Published
Have you ever struggled to fit medical appointments into your busy schedule? Has it been a challenge to keep up with medications and refills? Have you or a loved one had to travel a long way, sometimes repeatedly, to get treatment or see a provider?
If so, you’re not alone. Our healthcare system places burdens on patients at every turn. People must carve out time for exams, manage complex medication regimens, and make continual treks to doctor’s offices. The weight only grows for patients who live far from healthcare facilities or have limited resources.
When care doesn’t fit into patients’ lives, exams and vital treatments are missed. The results can be devastating—from preventable health crises to mounting expenses for both the patient and the healthcare system.
Our current care model means patients spend less time in their communities and more time traveling to clinics. But what if we had the power to break this pattern by allowing clinicians to remotely deliver essential care that continuously responds to a person’s unique biology directly into their bodies?
ARPA-H is making it possible.
With ARPA-H projects that push the state of the art of cell engineering and bioelectronics, Program Manager Paul E. Sheehan, Ph.D., envisions a convenient, affordable future of medicine where patients can receive critical health information and treatment through safe and secure devices that are worn, ingested, or implanted. Instead of care that constantly disrupts daily life, this technology will deliver care that works within it.
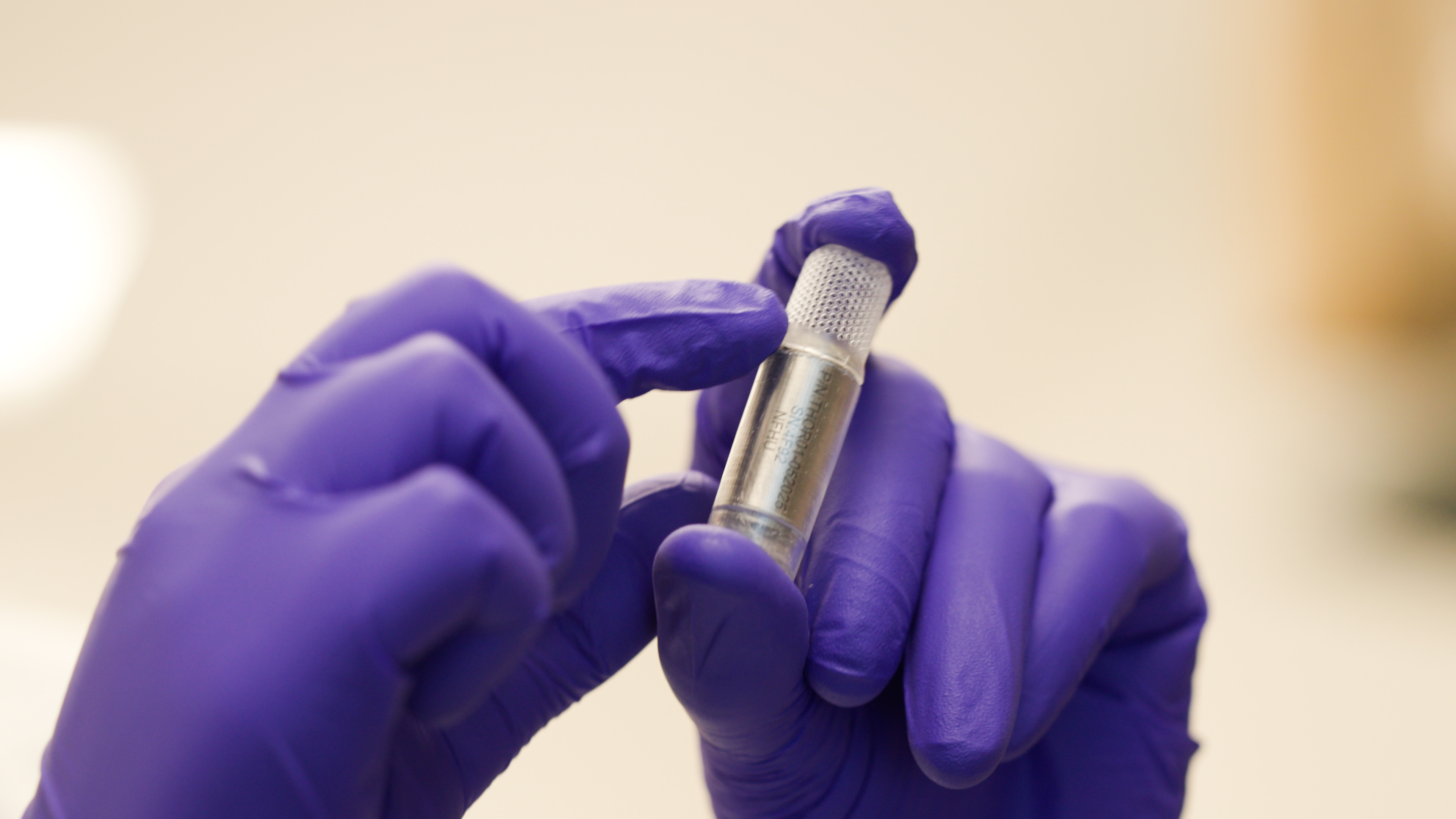
One innovative approach to cancer treatment called THOR (Targeted Hybrid Oncotherapeutic Regulation) is among the projects Dr. Sheehan oversees. THOR researchers at Rice University have created a small prototype implant designed to be placed near a patient’s tumor during a simple, outpatient surgery. Engineered cells within the device would then deliver therapeutic molecules directly to the tumor and surrounding tissue.
Unlike in a traditional chemotherapy clinic, clinicians could use the device’s smart sensors and control mechanisms to determine how well the treatment is working in real time and fine-tune dosing remotely. That means treatment can be adjusted without repeat trips or long days in waiting rooms so people with cancer could manage safe, cost-effective, personalized treatment from the comfort of their homes.
This reality is now one step closer as THOR performers launch a new biotech company to advance this technology to clinical trials in 2026.
Watch the video below to hear directly from Dr. Sheehan and THOR Principal Investigator Omid Veiseh, Ph.D.
Dr. Sheehan also oversees ARPA-H's Resilient Extended Automatic Cell Therapies (REACT) program, which aims to simplify arduous and expensive medication regimens for chronic illness by helping the body make its own medicine.
REACT research teams are currently developing implantable bioelectronic devices that use engineered cells to produce and deliver therapies for Inflammatory Bowel Disease (IBD), weight loss, diabetes, and hypothyroidism.
Like THOR, these implants would also sense and report indicators of treatment response and disease progress, so clinicians can fine-tune care remotely. If successful, this approach could replace trips to the pharmacy and prevent the costly down-stream effects of patients not taking medication as prescribed.

Most recently, ARPA-H and Dr. Sheehan launched the Delphi program, which aims to create discreet, low-cost wearable devices that sense deep biological information, like hormones and inflammatory markers. These advanced and affordable biosensors would move beyond tracking basics like heart rate. They would empower people to better understand their bodies, manage their health, and provide insights to help prevent disease—without the cost, hassle, and travel time of routine lab tests.
These patient-centered solutions point to a more affordable and accessible model of care that can reduce the hidden costs patients frequently absorb—like transportation, time off work, childcare, and missed opportunities to prevent or better manage illness.
While the bioelectronics and cell-engineering advances behind this technology are very new, the approach reflects the simplicity of an old-fashioned house call. In the future, care may once again come to the patient.
Dr. Sheehan is just one of many Program Managers transforming the future of health through their work with ARPA-H. Learn more about becoming an ARPA-H Program Manager.